The Natural History Database is a fantastic resource for research in TSC. It is an incredible resource for those in epidemiology, given its unparalleled size. It is an incredible resource for those with interests in basic sciences, including genetics, given the quality of the samples held in the Biosample Repository. I have had the opportunity to make use of both of these aspects and my efforts have been successful in no small part due to the support of the TSC Alliance.”
Mark Keezer, MDCM, PhD, Centre Hospitalier de l’Université de Montréal
Implemented in 2006, the TSC Natural History Database captures clinical data to document the impact of the disease on a person’s health over his or her lifetime. More than 2,700 people with TSC are enrolled in the project among 22 U.S.-based clinical sites. The TSC Alliance provides funding to participating clinics to perform data entry, monitors the integrity of the database, and makes data available to investigators to answer specific research questions and identify potential participants for clinical trials and studies. The TSC Alliance utilizes StudyTRAX as their platform to store and monitor Natural History Data.
Interested in requesting data from the TSC Natural History Database?
Please download and fill out this form then email it to Liz Cassidy, MPH, Research Project Manager, at ecassidy@tscalliance.org. All applications will be reviewed by the NHD-BSR Steering Committee.
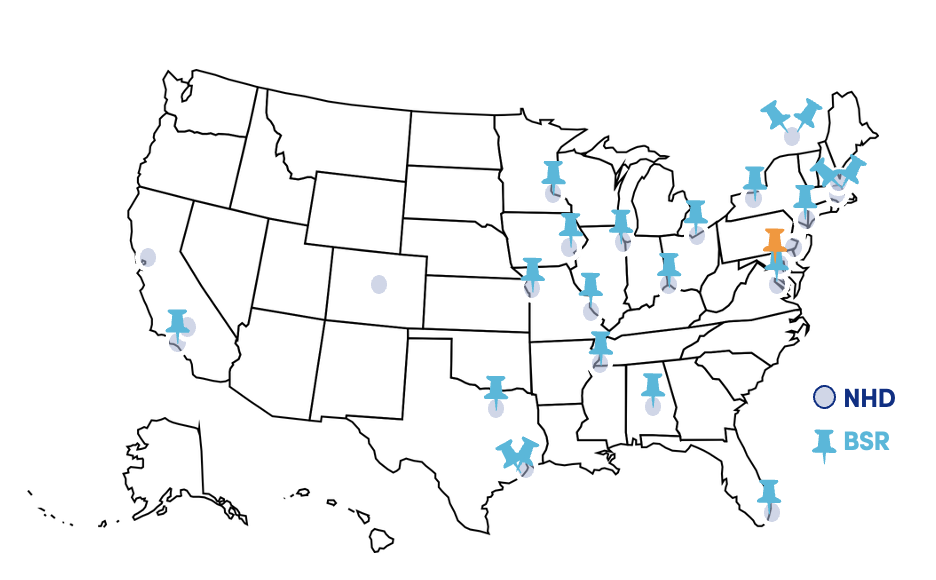
Current sites
Circle icons indicate a database only site meaning that biosamples are not collected on site. Pushpins indicate sites approved to collect biosamples on site
Publications
Since 2010, researchers have published various articles in well-regarded, peer-reviewed biomedical journals using data from the TSC Natural History Database. This published research has contributed to our understanding of TSC in a number of relevant fields, including neurology, psychiatry, and ophthalmology. Several papers have found correlations between gene mutations and specific TSC symptoms, as well as correlations between different kinds of symptoms. This type of work is helping us understand why and how different individuals with TSC experience the disease differently. Click the manifestations below to see publications using data from the Natural History Database.
Questions?
Contact biosample@tscalliance.org.
Information for individuals with TSC and their families
If you are an individual with TSC or a family member of someone with TSC, please see here for information about participating in the TSC Natural History Database.
Acknowledgments
The TSC Natural History Database and Biosample Repository are governed and wholly funded by the TSC Alliance thanks to generous support from Lorne Waxlax, William Watts, Dr. Michael and Janie Frost, Janice and Julian Gangolli Family Fund, Jim and the late Andrea Maginn, and many additional donors through the Unlock the Cure campaign.
Our thanks to UCB, Inc. for supporting translation of consent forms for this project into Spanish.
![]()