In a recent study, researchers investigated the immune microenvironment in Lymphangioleiomyomatosis (LAM), specifically focusing on macrophages, a type of immune cell, to explore potential targets for treatment. LAM, a rare, progressive lung disease, can occur in women with TSC and, sometimes in women without a TSC diagnosis. Current treatments can slow disease progression, but there is no cure.
Macrophages are a type of immune cell that ordinarily activates immune responses, allowing them to eliminate tumor cells, bacteria, and other foreign substances. Previous work had shown in angiomyolipomas, almost all of the macrophages have lost their ability to activate immune responses. These macrophages that suppress the immune system are often called M2 macrophages.
In new work, researchers found that most of the macrophages in LAM have features of M2 macrophages. They also used a specialized spatial profiling approach to discover that these M2 are found very close to LAM cells. The LAM cells near the macrophages make a signal called CXCL12 that could help attract macrophages. In the lab, when scientists grew human or mouse macrophages together with cells missing the TSC2 gene, the macrophages showed more M2 features.
The study reveals that macrophages are the most abundant immune cells in LAM-affected lung tissue:
- Immunosuppressive Nature: The majority of the macrophages in LAM exhibit what scientists call an immunosuppressive M2-like phenotype, characterized by expression of markers such as CD206. This M2-like phenotype is often associated with promoting tumor growth and progression in various cancers.
- Proximity to LAM Cells: Spatial analysis revealed that these M2-like macrophages are located in close proximity to LAM cells in human LAM lung specimens.
- LAM Cell Influence: Experiments in the laboratory demonstrated that TSC2-deficient LAM cells actively induce macrophages to adopt this immunosuppressive M2-like phenotype. This process may be driven by factors produced by LAM cells, such as CXCL12, which act to attract M2-like macrophages.
- Lung Tissue Destruction: LAM-associated macrophages located near cysts were found to express immunosuppressive genes and increased levels of cysteine proteases. Proteases break down lung tissue, suggesting that these macrophages could be involved lung tissue destruction.
Given the role of M2-like, CD206-positive macrophages in promoting LAM growth, the study explored targeting these cells as a potential therapeutic strategy using mice. The researchers used RP-182, a synthetic peptide that modulates CD206, to reprogram immunosuppressive macrophages into pro-inflammatory ones. In preclinical mouse models of LAM, treatment with RP-182 significantly restricted the growth of TSC2-deficient tumors. The data showed that RP-182 treatment reduced the number of CD206-positive macrophages in the tumors and enhanced the engulfment of tumor cells by M2-like macrophages.
This research highlights that immunosuppressive CD206-positive macrophages are abundant in LAM lungs and are actively recruited and influenced by LAM cells, contributing to disease progression and lung destruction. Targeting these macrophages, as demonstrated by the efficacy of RP-182 in mouse models of TSC, represents a promising novel therapeutic approach for LAM and TSC.
Lead author: Elizabeth P. Henske, MD, Director of the Center for LAM Research and Clinical Care at Brigham and Women’s Hospital, and Professor of Medicine at Harvard Medical School, Boston, MA
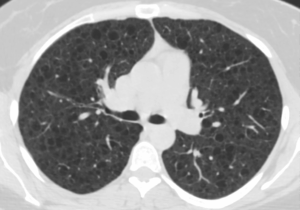
Image of lungs affected by Lymphangioleiomyomatosis (LAM) from The LAM Foundation.
Help the TSC Alliance accelerate TSC research by donating to the 50 Forward Fund!
